Arch Pain Triggers Warning Signs And Treatments
Overview
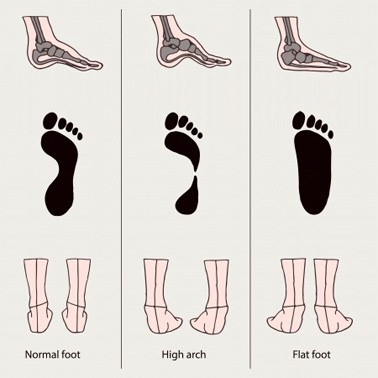
Flat feet are characterized by no arch in the inner foot. It can be a genetic condition or the result of improper body mechanics. Often the whole of the foot will contact the ground. A healthy foot structure supports the body's weight from the bone structure arch; a flat foot is unable to properly support this weight, causing pressure in the ankle, knee and hip joints.

Causes
Conditions that affect the nervous system (brain and spinal cord) can also cause the arches to fall. Over time, the muscles gradually become stiffer and weaker and lose their flexibility. Conditions where this can occur include cerebral palsy, spina bifida and muscular dystrophy. Adult-acquired flat feet often affect women over 40 years of age. It often goes undiagnosed and develops when the tendon that supports the foot arch gradually stretches over time. It's not fully understood what causes the tendon to become stretched, but some experts believe that wearing high heels and standing or walking for long periods may play a part. Obesity, high blood pressure (hypertension) and diabetes are all risk factors.
Symptoms
If you've ever seen your footprints in the sand and they looked more like bricks than feet, then you probably have flat feet. Simply stated, a flat foot is a foot that does not have an arch when standing. In the medical world, flat feet are associated with "pronated" feet. Pronated is merely the term used to describe the position of the foot when it is flexed upward (dorsiflexed), turned away from the body (abducted), and the heel is rolled outward (everted), all at the same time. A certain amount of pronation is required for normal walking, but too much pronation is often considered a foot's "worst enemy." Over time, excessive pronation can lead to many unpleasant problems including heel pain, bunions, hammertoes, shin splints, and even knee, hip, or back pain. In fact, one orthopedic surgeon discovered that 95% of his total knee replacement patients and 90% of his total hip replacement patients had flat feet. An easy way to tell if you pronate too much is to take a look at your athletic shoes-excessive wearing of the inside heel (arch side of the shoe) as compared to the outside is a classic indication of excessive pronation.
Diagnosis
A professional therapist may use tinels test to diagnose tarsal tunnel syndrome. This involves tapping the nerve just behind the medial malleolus or bony bit of the ankle with a rubber hammer. Pain indicates a positive test. Sometimes it is initially mistaken for plantar fasciitis which also causes pain from the inside heel and throughout the arch of the foot. Neural symptoms (such as tingling or numbness) as well as the location of tenderness when touching the area should help to easily distinguish between the conditions.
Non Surgical Treatment
Treatment of plantar fasciitis is sometimes a drawn out and frustrating process. A program of rehabilitation should be undertaken with the help of someone qualified and knowledgeable about the affliction. Typically, plantar fasciitis will require at least six weeks and up to six months of conservative care to be fully remedied. Should such efforts not provide relief to the athlete, more aggressive measures including surgery may be considered. The initial goals of physical therapy should be to increase the passive flexion of the foot and improve flexibility in the foot and ankle, eventually leading to a full return to normal function. Prolonged inactivity in vigorous sports is often the price to be paid for thorough recovery. Half measures can lead to a chronic condition, in some cases severely limiting athletic ability.
Surgical Treatment
With flat feet, there is a tendon on the inside of the foot than can often become weakened, injured, split and/or ruptured. This tendon, is called the posterior tibial tendon, and is the main arch supporting tendon. Obviously damage to this tendon can cause collapse of the arch. Some people have genetically inefficient tendon, and tends to be the case in younger people. In mild cases, such as tendon splits, the posterior tibial tendon can be repaired to restore its strength. Acute incontinuity of the tendon can be primarily repaired. Often the posterior tibial tendon is augmented with a tendon transfer of an adjacent tendon to provide both strength and continuity. In any tendon repair, advanced or retensioning of the tendon is performed. In most flat foot surgery a tendon augmentation is often combined with other boney procedures to restore structure and balance to the foot.
Stretching Exercises
You may start exercising the muscles of your foot right away by gently stretching and strengthening them. Frozen can roll. Roll your bare injured foot back and forth from your heel to your mid-arch over a frozen juice can. Repeat for 3 to 5 minutes. This exercise is particularly helpful if it is done first thing in the morning. Towel stretch. Sit on a hard surface with your injured leg stretched out in front of you. Loop a towel around your toes and the ball of your foot and pull the towel toward your body keeping your leg straight. Hold this position for 15 to 30 seconds and then relax. Repeat 3 times. Standing calf stretch. Stand facing a wall with your hands on the wall at about eye level. Keep your injured leg back with your heel on the floor. Keep the other leg forward with the knee bent. Turn your back foot slightly inward (as if you were pigeon-toed). Slowly lean into the wall until you feel a stretch in the back of your calf. Hold the stretch for 15 to 30 seconds. Return to the starting position. Repeat 3 times. Do this exercise several times each day. Seated plantar fascia stretch. Sit in a chair and cross the injured foot over the knee of your other leg. Place your fingers over the base of your toes and pull them back toward your shin until you feel a comfortable stretch in the arch of your foot. Hold 15 seconds and repeat 3 times. Plantar fascia massage. Sit in a chair and cross the injured foot over the knee of your other leg. Place your fingers over the base of the toes of your injured foot and pull your toes toward your shin until you feel a stretch in the arch of your foot. With your other hand, massage the bottom of your foot, moving from the heel toward your toes. Do this for 3 to 5 minutes. Start gently. Press harder on the bottom of your foot as you become able to tolerate more pressure.
Flat feet are characterized by no arch in the inner foot. It can be a genetic condition or the result of improper body mechanics. Often the whole of the foot will contact the ground. A healthy foot structure supports the body's weight from the bone structure arch; a flat foot is unable to properly support this weight, causing pressure in the ankle, knee and hip joints.

Causes
Conditions that affect the nervous system (brain and spinal cord) can also cause the arches to fall. Over time, the muscles gradually become stiffer and weaker and lose their flexibility. Conditions where this can occur include cerebral palsy, spina bifida and muscular dystrophy. Adult-acquired flat feet often affect women over 40 years of age. It often goes undiagnosed and develops when the tendon that supports the foot arch gradually stretches over time. It's not fully understood what causes the tendon to become stretched, but some experts believe that wearing high heels and standing or walking for long periods may play a part. Obesity, high blood pressure (hypertension) and diabetes are all risk factors.
Symptoms
If you've ever seen your footprints in the sand and they looked more like bricks than feet, then you probably have flat feet. Simply stated, a flat foot is a foot that does not have an arch when standing. In the medical world, flat feet are associated with "pronated" feet. Pronated is merely the term used to describe the position of the foot when it is flexed upward (dorsiflexed), turned away from the body (abducted), and the heel is rolled outward (everted), all at the same time. A certain amount of pronation is required for normal walking, but too much pronation is often considered a foot's "worst enemy." Over time, excessive pronation can lead to many unpleasant problems including heel pain, bunions, hammertoes, shin splints, and even knee, hip, or back pain. In fact, one orthopedic surgeon discovered that 95% of his total knee replacement patients and 90% of his total hip replacement patients had flat feet. An easy way to tell if you pronate too much is to take a look at your athletic shoes-excessive wearing of the inside heel (arch side of the shoe) as compared to the outside is a classic indication of excessive pronation.
Diagnosis
A professional therapist may use tinels test to diagnose tarsal tunnel syndrome. This involves tapping the nerve just behind the medial malleolus or bony bit of the ankle with a rubber hammer. Pain indicates a positive test. Sometimes it is initially mistaken for plantar fasciitis which also causes pain from the inside heel and throughout the arch of the foot. Neural symptoms (such as tingling or numbness) as well as the location of tenderness when touching the area should help to easily distinguish between the conditions.
Non Surgical Treatment
Treatment of plantar fasciitis is sometimes a drawn out and frustrating process. A program of rehabilitation should be undertaken with the help of someone qualified and knowledgeable about the affliction. Typically, plantar fasciitis will require at least six weeks and up to six months of conservative care to be fully remedied. Should such efforts not provide relief to the athlete, more aggressive measures including surgery may be considered. The initial goals of physical therapy should be to increase the passive flexion of the foot and improve flexibility in the foot and ankle, eventually leading to a full return to normal function. Prolonged inactivity in vigorous sports is often the price to be paid for thorough recovery. Half measures can lead to a chronic condition, in some cases severely limiting athletic ability.

Surgical Treatment
With flat feet, there is a tendon on the inside of the foot than can often become weakened, injured, split and/or ruptured. This tendon, is called the posterior tibial tendon, and is the main arch supporting tendon. Obviously damage to this tendon can cause collapse of the arch. Some people have genetically inefficient tendon, and tends to be the case in younger people. In mild cases, such as tendon splits, the posterior tibial tendon can be repaired to restore its strength. Acute incontinuity of the tendon can be primarily repaired. Often the posterior tibial tendon is augmented with a tendon transfer of an adjacent tendon to provide both strength and continuity. In any tendon repair, advanced or retensioning of the tendon is performed. In most flat foot surgery a tendon augmentation is often combined with other boney procedures to restore structure and balance to the foot.
Stretching Exercises
You may start exercising the muscles of your foot right away by gently stretching and strengthening them. Frozen can roll. Roll your bare injured foot back and forth from your heel to your mid-arch over a frozen juice can. Repeat for 3 to 5 minutes. This exercise is particularly helpful if it is done first thing in the morning. Towel stretch. Sit on a hard surface with your injured leg stretched out in front of you. Loop a towel around your toes and the ball of your foot and pull the towel toward your body keeping your leg straight. Hold this position for 15 to 30 seconds and then relax. Repeat 3 times. Standing calf stretch. Stand facing a wall with your hands on the wall at about eye level. Keep your injured leg back with your heel on the floor. Keep the other leg forward with the knee bent. Turn your back foot slightly inward (as if you were pigeon-toed). Slowly lean into the wall until you feel a stretch in the back of your calf. Hold the stretch for 15 to 30 seconds. Return to the starting position. Repeat 3 times. Do this exercise several times each day. Seated plantar fascia stretch. Sit in a chair and cross the injured foot over the knee of your other leg. Place your fingers over the base of your toes and pull them back toward your shin until you feel a comfortable stretch in the arch of your foot. Hold 15 seconds and repeat 3 times. Plantar fascia massage. Sit in a chair and cross the injured foot over the knee of your other leg. Place your fingers over the base of the toes of your injured foot and pull your toes toward your shin until you feel a stretch in the arch of your foot. With your other hand, massage the bottom of your foot, moving from the heel toward your toes. Do this for 3 to 5 minutes. Start gently. Press harder on the bottom of your foot as you become able to tolerate more pressure.